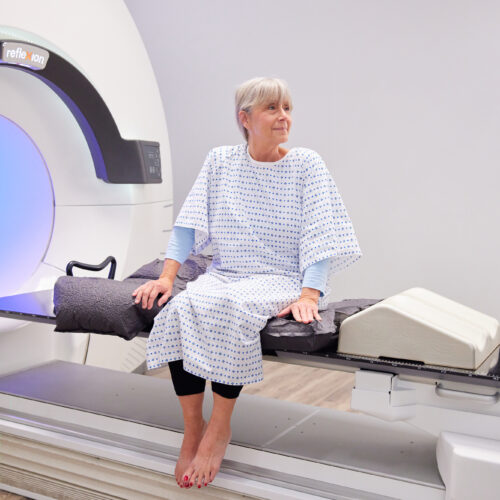
BgRT
Combination Therapies in the Fight Against Cancer – Sometimes the Best Medicine is All of Them
September 30, 2021
Cancer is a frightening disease and a serious medical problem that does not discern age, sex, race, ethnicity, or socio-economic status. Despite significant gains in understanding and treating cancer over the past 100 years, cancer has become efficient at avoiding detection and physically changing to escape the treatments we’ve used to destroy it. The American Cancer Society estimates in the U.S. alone, almost two million Americans will be diagnosed with cancer in 2021. And currently annual mortality from cancer stands at over 600,000 people.1
Three leading cancers—breast, lung and prostate—will account for nearly one-third of the almost two million total cancer cases in the U.S. These numbers are sobering. People may ask, with all the money and support given to cancer research, why can’t we beat cancer once and for all? What will it take to eradicate this dreadful disease?
The improvement in outcomes is also due to better screening procedures to detect disease at an earlier stage, improved and customizable treatment options, new diagnostic tests, and advanced imaging in evaluating the spread of disease. Additionally, we are seeing promising advances in controlling cancer and extending lives with new combination therapies.
Combination therapy combines two or more therapies to treat cancer. Emil Frei, James F. Holland and Emil J. Freireich first conceptualized combination therapy in 1965.3 They postulated the first-ever combination therapy to treat acute leukemia.3 Today, whether it is a combination of different drugs, or different treatment modalities like surgery and chemotherapy, or immunotherapy and radiotherapy, or radiopharmaceutical therapy with drug therapy, physicians use combination therapy to attack the cancer on different fronts—namely, by disabling the cancer’s escape mechanisms, shutting down its ability to resist drugs, choking off its blood supply or permanently damaging its DNA so it cannot reproduce.
Currently, there are more than 386,000 clinical trials open globally,125,000 of which are in the U.S., and about 2,300 of which are devoted to oncology.4 With so many clinical trials investigating different treatments for cancers, it can be overwhelming for patients and their families to decide which trial to participate in.
For example, here are some recent U.S. clinical trial results and open trials that involve combination therapy or compare therapies in the fight against the three most common cancers:
LUNG
Recent results from the Checkmate-816 study reveal neoadjuvant (i.e., treatment given before surgery to decrease the tumor’s size) nivolumab (immunotherapy) + chemotherapy produce substantial reductions in tumor size, compared to treatment with chemotherapy only. Patients who received this combination therapy subsequently had surgery to remove the entire tumor.5 ClinicalTrials.gov Identifier: NCT02998528
The STARS study examined stereotactic ablative radiotherapy (SABR) in comparison to video-assisted thoracic surgery (VATS) and found using SABR in patients with Stage I non-small cell lung cancer (NSCLC) is a viable therapeutic option in place of surgery. Results of treatment from SABR are similar or superior to VATS and may be a great option for non-invasive treatment in patients where surgery would be contraindicated due to health conditions.5 ClinicalTrials.gov Identifier: NCT02357992
The PACIFIC trial five-year data documents continuing benefits in patients with unresectable Stage III NSCLC who were treated with concurrent chemo-radiotherapy + Durvalumab (immunotherapy) versus treatment using a placebo. Investigators estimated that 43 percent of patients randomized to Durvalumab are living after five years and about one-third of those patients remain progression free.5 ClinicalTrials.gov Identifier: NCT02125461
BREAST
The Phase 3 OlympiA clinical trial results revealed one year of adjuvant Olaparib (Lynparza) (non-chemotherapy oral medication) can undoubtedly diminish the risk of the cancer returning and avert metastasis in women with high-risk, early-stage, HER2-negative breast cancer who have an inherited BRCA1 or BRCA2 gene mutation. Adjuvant treatment is the therapy given after the main treatment. Metastasis is cancer that has spread to another part of the body.6
Open Trial: Olaparib Concurrently with Radiotherapy vs. Radiotherapy Alone in Treating Patients with Inflammatory Breast Cancer. The purpose of this study is to evaluate how well radiation therapy with or without Olaparib (Lynparza) works in treating patients with inflammatory breast cancer. Radiation therapy uses high-energy x-rays to kill tumor cells and shrink tumors. Olaparib may stop the growth of tumor cells by blocking some of the enzymes needed for cell growth. It is not yet known whether radiation therapy with or without Olaparib may work better in treating patients with inflammatory breast cancer.7
PROSTATE
The Phase 3 VISION Clinical Trial demonstrates that a radiopharmaceutical treatment named lutetium-177-PSMA-617 (177Lu-PSMA-617 or LuPSMA), when given concurrently with standard of care treatments, impedes the proliferation of metastatic castrate-resistant prostate cancer (mCRPC) several months longer than standard of care treatment and helps people live around four months longer over standard of care therapy alone.6
Open Trial: Antiandrogen Therapy and Radiation Therapy With or Without Docetaxel in Treating Patients with Prostate Cancer That Has Been Removed by Surgery. This randomized Phase II/III trial studies Docetaxel (chemotherapy drug), anti-androgen therapy (hormone therapy) and radiation therapy to see how well it works compared with anti-androgen therapy and radiation therapy alone in treating patients with prostate cancer that has been removed by surgery. Androgen can cause the growth of prostate cells. Anti-hormone therapy may lessen the amount of androgen made by the body. Radiation therapy uses high-energy x-rays to kill tumor cells and shrink tumors. Drugs used in chemotherapy, such as Docetaxel, work in different ways to stop the growth of tumor cells, either by killing the cells, or by stopping them from dividing or spreading. Giving anti-androgen therapy and radiation therapy with or without Docetaxel after surgery may kill any remaining tumor cells.8
Research into combination therapies shows great promise in improving outcomes for people with cancer while maintaining their quality of life. By its very nature, cancer will continue to adapt and evolve, but so will medical research change and advance to make cancer a more treatable disease rather than a terminal one. Combination therapies may be the best arsenal yet in the fight against cancer.
References
- Siegel, R. L., Miller, K. D., Fuchs, H. E., and Jemal, A. (2021). Cancer Statistics, 2021. CA: A Cancer Journal for Clinicians. 71(1): 7–33. https://doi.org/10.3322/caac.21654
- Retrieved from https://seer.cancer.gov/
- Mokhtari, R. B., Homayouni, T. S., Baluch, N., et al. (2017). Combination therapy in combating cancer. Oncotarget. 8(23):38022–28043. Doi: 10.18632/oncotarget.16723
- Retrieved from https://clinicaltrials.gov/
- Kunde, J. ASCO 2021: Progress in Lung Cancer Treatment. June 11, 2021. https://www.lungevity.org/blogs/asco-2021-progress-in-lung-cancer-treatment
- ASCO Staff. Olaparib reduces risk of recurrence and metastasis in people with a BRCA mutation and early-stage, HER2-negative breast cancer. Cancer.net. June 3, 2021. https://www.cancer.net/blog/2021-06/2021-asco-annual-meeting-new-treatments-and-research-advances-esophageal-cancer-prostate-cancer#breast
- Mayo Clinic. 2021. A Study to Compare Administering Olaparib Concurrently With Radiotherapy vs. Radiotherapy Alone in Treating Patients With Inflammatory Breast Cancer. https://www.mayo.edu/research/clinical-trials/cls-20455751
- ClinicalTrials.gov. 2021. Anti-androgen Therapy and Radiation Therapy With or Without Docetaxel in Treating Patients With Prostate Cancer That Has Been Removed by Surgery. https://clinicaltrials.gov/ct2/show/NCT03070886